
Biography
Biography: Anupam Gupta
Abstract
Introduction: Preterm infants often require mechanical ventilation. Volume targeted ventilation has been shown to reduce both complications and the duration of mechanical ventilation. Recommended tidal volume varies from 4-8 mL/kg, but the optimal tidal volume remains elusive.
Aim: To compare a lower (4-5 mL/kg) to a higher (7-8 mL/kg) tidal volume during Volume Guarantee ventilation (VG) of Respiratory Distress Syndrome (RDS) in very preterm infants.
Method: The randomized trial was conducted at North Tees Hospital from 2013-2016. Babies <32 weeks’ gestation or <1500 grams birthweight and requiring mechanical ventilation within 12 hours of life from RDS were included in the study. Babies were randomized to receive lower (4-5 mL/kg) or higher (7-8 mL/kg) tidal volume using VG. The dead space was kept consistent by using standardized trimming of the ET tube. Subjects all received surfactant and were managed by a strict protocol with rescue by high frequency ventilation for defined criteria. The primary outcome was the time to achieve a 25% reduction from the initial Peak Inspiratory Pressure (PIP). Secondary outcomes included the duration of mechanical ventilation, as well as respiratory and nonrespiratory complications. The data were analyzed using SPSS® version 20.0.
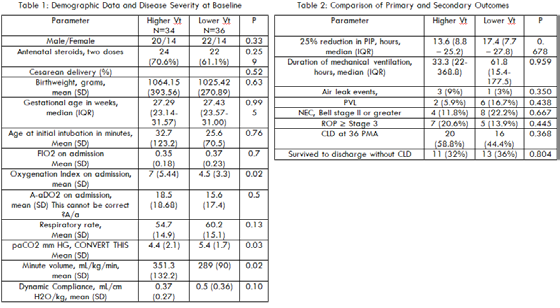
Result: During the study period, 70 of 97 (72%) eligible infants were enrolled. The groups were similar (Table 1). The primary outcome, time to reduce PIP (median [IQR]) were 13.6 (8.8-25.2) hours and 17.4 (7.7-27.8) hours, respectively, for higher and lower Vt (p=0.678). The total duration of ventilation (median [IQR]) on higher vs. lower tidal volume was 33.3 (22-368.8) and 61.8 (15.4-177.5) hours, respectively (p=0.959). There were no differences between the two groups for respiratory and non-respiratory complications of prematurity (Table 2).
Conclusion: This study failed to find differences in lower versus higher tidal volume delivery in a small population of infants with RDS. It is possible that both tidal volume ranges selected for study are at functional residual capacity.

